“We are committed to provide Quality Unani and Ayurvedic medicinal formulations!!!”

What is diabetes ?
Diabetes is a condition in which there is too much glucose (a sugar that is the body’s main source of energy) in the blood. If undetected or not controlled, diabetes can cause complications both in the short term (including increased risk of infections) and long term (see below).
Diabetes develops when the pancreas, the gland that makes insulin, is either unable to make insulin or the insulin does not work properly. Without enough insulin (a hormone that lowers glucose levels in the blood) blood glucose levels rise and lead to health problems.
What are the different types of diabetes ?
There are two main types of diabetes. Type 1 diabetes can begin at any age but often starts in childhood or young adulthood. A person with type 1 diabetes cannot make enough insulin and must have insulin every day to live. About 85 per cent of people with diabetes have type 2 diabetes, which is linked to diet, lack of exercise, obesity and family history. A person with type 2 diabetes does not produce enough insulin to control their blood glucose levels.
Diabetes mellitus is a disease caused by deficiency or diminished effectiveness of endogenous insulin. It is characterised by hyperglycaemia, deranged metabolism and sequelae predominantly affecting the vasculature.
The main types of diabetes mellitus are :
Type 1 diabetes mellitus: results from the body's failure to produce sufficient insulin.
Type 2 diabetes mellitus: results from resistance to the insulin, often initially with normal or increased levels of circulating insulin.
Gestational diabetes: pregnant women who have never had diabetes before but who have high blood glucose levels during pregnancy are said to have gestational diabetes. Gestational diabetes affects about 4% of all pregnant women. It may precede development of type 2 (or rarely type 1) diabetes.
Maturity-onset diabetes of the young (MODY) includes several forms of diabetes with monogenetic defects of beta-cell function (impaired insulin secretion), usually manifesting as mild hyperglycaemia at a young age, and usually inherited in an autosomal-dominant manner.
Secondary diabetes: accounts for only 1-2% of patients with diabetes mellitus.
Causes include :
Pancreatic disease: cystic fibrosis, chronic pancreatitis, pancreatectomy, carcinoma of the pancreas.
Endocrine: Cushing's syndrome, acromegaly, thyrotoxicosis, phaeochromocytoma, glucagonoma
Drug-induced: thiazide diuretics, corticosteroids, atypical antipsychotics, antiretroviral protease inhibitors.
Congenital lipodystrophy.
Acanthosisnigricans.
Genetic: Wolfram's syndrome (which is also referred to as DIDMOAD: diabetes insipidus, diabetes mellitus, optic atrophy and deafness),Friedreich's ataxia, dystrophiamyotonica, haemochromatosis, glycogen storage diseases.
Some patients with type 2 diabetes require insulin, so the old terms of insulin-dependent diabetes mellitus (IDDM) for type 1 diabetes and non-insulin-dependent diabetes mellitus (NIDDM) for type 2 diabetes are inappropriate. Type 2 diabetes is increasingly diagnosed in children and adolescents and so the old term maturity-onset diabetes for type 2 diabetes is also inappropriate.
Can diabetes be prevented ?
Type 1 diabetes cannot be prevented. However, type 2 diabetes may be prevented by a healthy lifestyle including regular physical activity, a healthy diet and keeping weight in the healthy range. Visit the Diabetes Australia website (www.diabetesaustralia.com.au) for more general information about diabetes and its treatment.
What health problems are caused by diabetes ?
If undetected or poorly controlled, diabetes can lead to a shorter life. Diabetes can cause blindness, kidney failure, nerve damage, reduced blood circulation that may lead to lower limb amputation, and can increase the chance of cardiovascular disease (heart attack and stroke). Men with diabetes also have a higher chance of developing sexual and reproductive health problems including :
erectile dysfunction
androgen (or testosterone) deficiency
low libido (sexual desire)
retrograde ejaculation (semen flows back into the bladder)
balanitis (inflammation of the head of the penis)
Type 1 diabetes mellitus
The development of type 1 diabetes mellitus is based on a combination of a genetic predisposition and an autoimmune process that results in gradual destruction of the beta cells of the pancreas, leading to absolute insulin deficiency. There is usually a pre-diabetic phase where autoimmunity has already developed but with no clinically apparent insulin dependency. Insulin autoantibodies can be detected in genetically predisposed individuals as early as 6-12 months of age. Possible triggers for the process may include viruses, dietary factors, environmental toxins, and emotional or physical stress. Early cessation of breast-feeding has also been linked to increased risk of developing type 1 diabetes, but the association is unproven and controversial.
Approximately 15% of those with diabetes have type 1 diabetes - usually juvenile-onset, but it may occur at any age. It may be associated with other autoimmune diseases. It is characterised by insulin deficiency.
There is 30-50% concordance in identical twins and a positive family history in 10% of people with type 1 diabetes. Screening for the diagnosis of diabetes in first-degree relatives of patients with type 1 is therefore reasonable, keeping in mind that the absolute risk is quite low.
Associated with HLA DR3 and DR4 and islet cell antibodies around the time of diagnosis.
Patients always need insulin treatment and are prone to ketoacidosis.
The most at-risk population for type 1 diabetes is Caucasian of northern European ancestry. Incidence is high in Scandinavian people.
Type 2 diabetes mellitus
Approximately 85% of those with diabetes; they are usually older at presentation (usually >30 years of age) but it is increasingly diagnosed in children and adolescents.Type 2 diabetes is associated with excess body weight and physical inactivity.All racial groups are affected but there is increased prevalence in people of South Asian, African, African-Caribbean, Polynesian, Middle-Eastern and American-Indian ancestry.It is caused by impaired insulin secretion and insulin resistance and has a gradual onset.Those with type 2 diabetes may eventually need insulin treatment.
Prevalence
In 2011 there were 2.9 million people with diabetes. It is estimated that 5 million people will have diabetes in the UK by 2025.It is estimated that there are around 850,000 people in the UK who have diabetes but have not been diagnosed.The UK average prevalence of diabetes in the UK is 4.45% but there are variations between countries and regions.The proportion of people with diabetes increases with age.
However, the incidence of diabetes is increasing in all age groups. Type 1 diabetes is increasing in children (especially those aged < 5 years), and type 2 diabetes is increasing, particularly in black and minority ethnic groups.
Risk factors for type 2 diabetes.
Obesity, especially central (truncal) obesity.
Lack of physical activity.
Ethnicity: people of South Asian, African, African-Caribbean, Polynesian, Middle-Eastern and American-Indian descent are at greater risk of type 2 diabetes, compared with the white population.
History of gestational diabetes.
Impaired glucose tolerance.
Impaired fasting glucose.
Drug therapy - eg, combined use of a thiazide diuretic with a beta-blocker.
Low-fibre, high-glycaemic index diet.
Metabolic syndrome.
Polycystic ovarian syndrome.
Adults who had low birth weight for gestational age.
Presentation
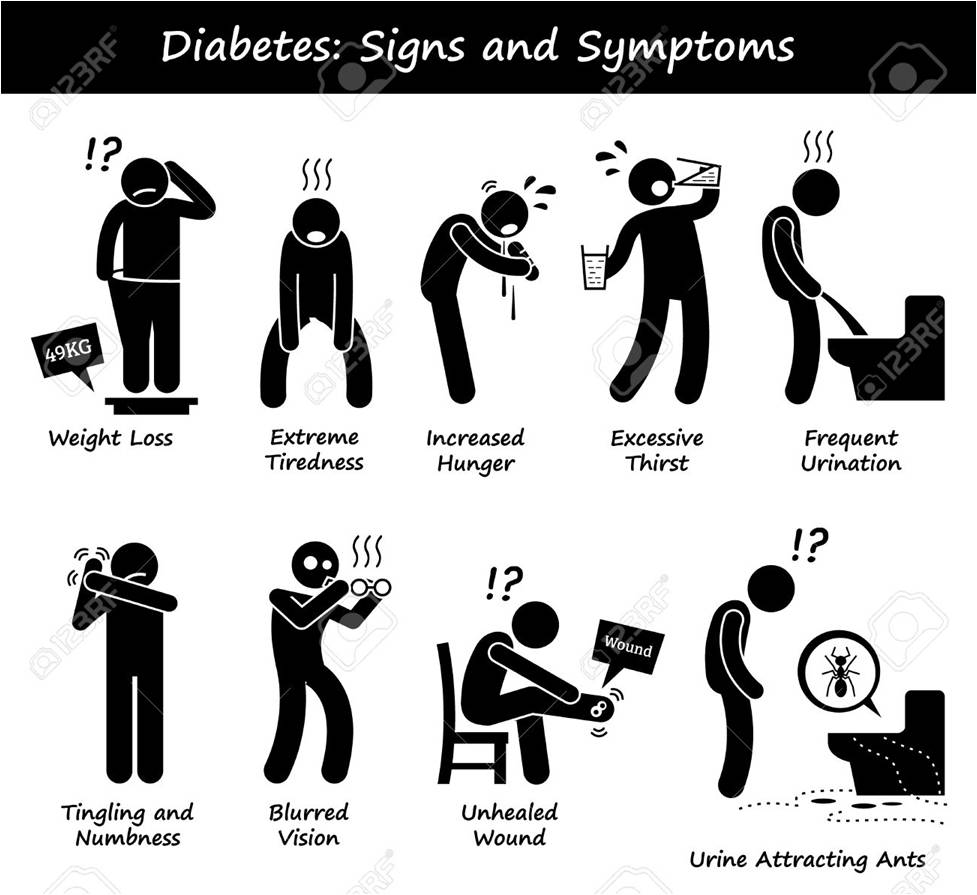
Patients with all types of diabetes may present with polyuria, polydipsia, lethargy, boils, pruritus vulvae or with frequent, recurrent or prolonged infections. Patients with type 1 diabetes may also present with weight loss, dehydration, ketonuria and hyperventilation. Presentation of type 1 diabetes tends to be acute with a short duration of symptoms.Presentation in patients with type 2 diabetes tends to be subacute with a longer duration of symptoms.Patients with diabetes may present with acute or chronic complications, as outlined in the section 'Complications', below.
Diagnosis
Diabetes may be diagnosed on the basis of one abnormal plasma glucose (random ≥11.1 mmol/L or fasting ≥7 mmol/L) in the presence of diabetic symptoms such as thirst, increased urination, recurrent infections, weight loss, drowsiness and coma.
In asymptomatic people with an abnormal random plasma glucose, two fasting venous plasma glucose samples in the abnormal range (≥7 mmol/L) are recommended for diagnosis.
Two-hour venous plasma glucose concentration ≥11.1 mmol/L two hours after 75 g anhydrous glucose in an oral glucose tolerance test (OGTT).
The World Health Organization (WHO) now recommends that glycatedhaemoglobin (HbA1c) can be used as a diagnostic test for diabetes. An HbA1c of 48 mmol/mol (6.5%) is recommended as the cut-off point for diagnosing diabetes. A value less than 48 mmol/mol does not exclude diabetes diagnosed using glucose tests.[7] See also the separate article on GlycatedHaemoglobin.
Management
The management plan for a person with diabetes includes
Diabetes education: structured education and self-management (at diagnosis and regularly reviewed and reinforced) to promote awareness.
Diet and lifestyle: healthy diet, weight loss if the person is overweight, smoking cessation, regular physical exercise.
Maximising glucose control while minimising adverse effects of treatment, such as hypoglycaemia.
Reduction of other risk factors for complications of diabetes, including the early detection and management of hypertension, drug treatment to modify lipid levels and consideration of antiplatelet therapy with aspirin.
Monitoring and early intervention for complications of diabetes, including cardiovascular disease, feet problems, eye problems, kidney problems and neuropathy.



